
Dr. Yingzi Yang, professor of Developmental Biology and associate dean for Research, and Dr. Jennifer Gibbs, assistant professor of Restorative Dentistry and Biomaterials Sciences and program director for Endodontics, have been awarded $200,000 in seed grant funding from the Harvard Stem Cell Institute to investigate how stem cells could play a role in repairing dentin and preserving dental pulp. Their work may offer new biological solutions for those suffering from debilitating dental pain that can occur with deep cavities.
“As dental cavities progress into the innervated vital pulp, pain and dangerous oral infections can occur,” said Gibbs. “In early studies we’ve seen the potential to identify new signaling pathways to enhance protective dentin formation that could lead to future treatments for biologically-based tooth repair.”
Their study seeks to identify and characterize the dental pulp stem cells (DPSCs) responsible for dentin repair in molar teeth and determine the effect of tooth injury on the expression of Sonic hedgehog (Shh) protein and other reparative signaling factor(s) that can be released from the neurons innervating the dental pulp. The same neurons that can cause pain, when activated can release substances, like Shh, which signal to DPSCs, potentially inducing repair and regeneration of dental pulp and dentin.
“The dental pulp is unique in its capacity for regeneration due to DPSCs. It is densely innervated with sensory neuron afferents, which play a critical role in pulp survival by sensing infection and damage,” said Yang. “Despite the importance of DPSCs and sensory neurons in pulpitis and injury repair, how their regulation can be harnessed to regenerate dentin in vivo remains a critical knowledge gap. Our objective is to identify mechanisms whereby the innervated murine molar dental pulp senses and responds to dentin damage.”
Yang and Gibbs began their collaboration two years ago. Recognizing that tooth pain after dental cavities or tooth fracture is a common problem in dentistry, their interests in dental regenerative medicine, and complimentary research expertise in the Yang and Gibbs labs, led them to test the hypothesis that pain sensation plays a critical role in injury repair by regulating stem cells.
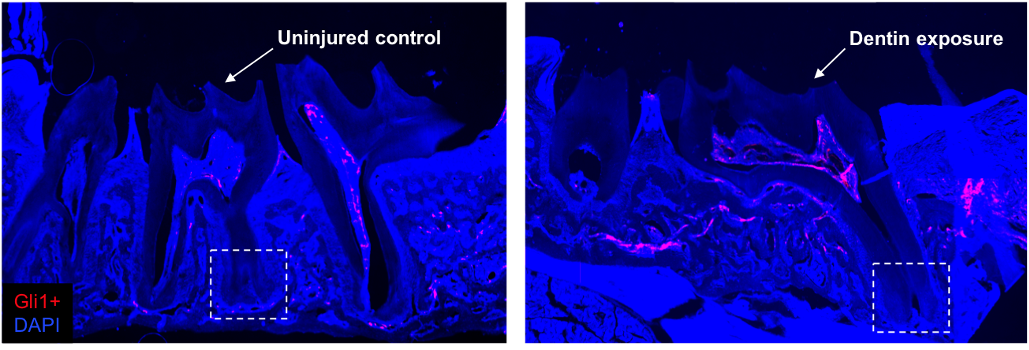
Postdoctoral scholars Dr. Emily Moore, previously of Dr. Yang’s lab, and Dr. Benoit Michot, of Dr. Gibbs’ lab, were critical to conducting the foundational experiments in support of this hypothesis. The researchers proposed that sensory neurons are critical regulators of stem cell activity and immunological signaling in the dental pulp affected by deep caries. The densely innervated dental pulp has an unparalleled capacity to transmit pain and teeth that have the neurons removed have more rapid progression of pathology in animal tooth injury models. Their hypothesis is derived from compelling preliminary data that activated sensory neurons induce Hedgehog signaling and inflammatory gene expression in murine molar pulp cells. Sonic Hedgehog and calcitonin gene related peptide, an important neuropeptide, both are intriguing targets for activation of stem cells in the dental pulp.
“This has been a terrific collaboration, allowing for the bridging between clinical and basic science expertise. It’s wonderful to be supported by the Harvard Stem Cell Institute to further pursue this work,” said Gibbs.
Their research could help identify previously uncharacterized stem cells for natural repair in the molar and novel therapeutic targets to treat dental pain and inflammation while enhancing endogenous mechanisms of dentin repair.
“We’re excited to see where this research will lead,” Yang and Gibbs said. “The ultimate goal of this work would be to reduce painful infections and costly interventions and optimize tooth retention.”


